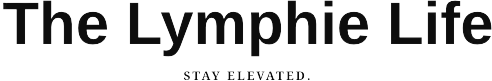Cancer Patients
and Survivors
Compassionate, evidence-informed nutrition to support your treatment and recovery, from an expert who’s been where you are.


Learn the top 7 nutrition strategies
to manage your lymphedema.


Customizable teaching tool template
to use with your patients.

Lymphedema Diet

Herbs for Lymphedema
Products for Lymphedema
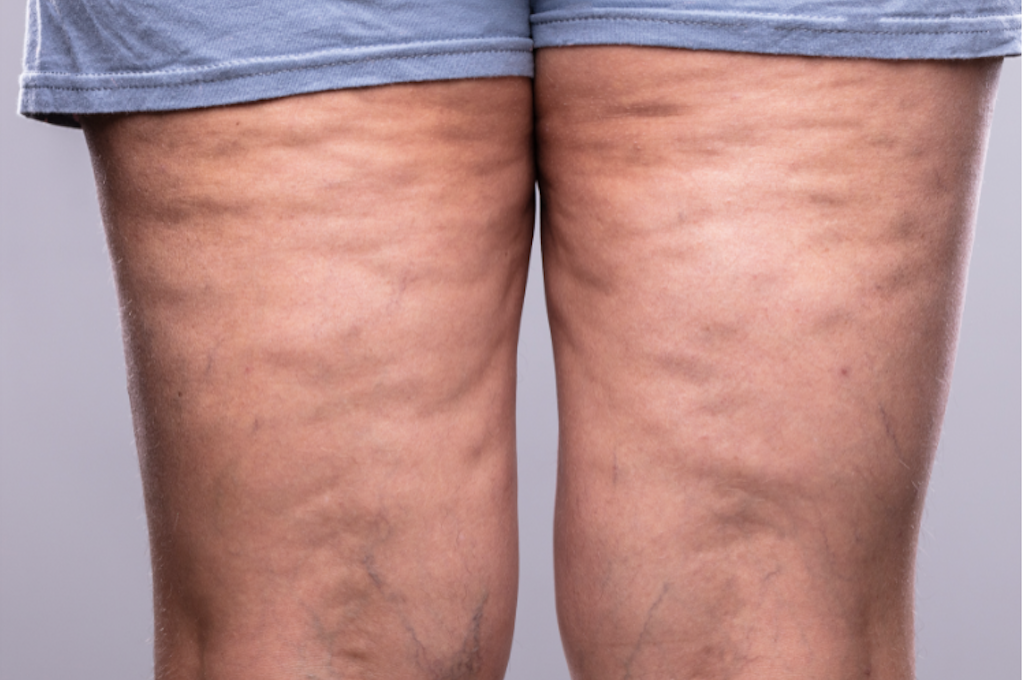
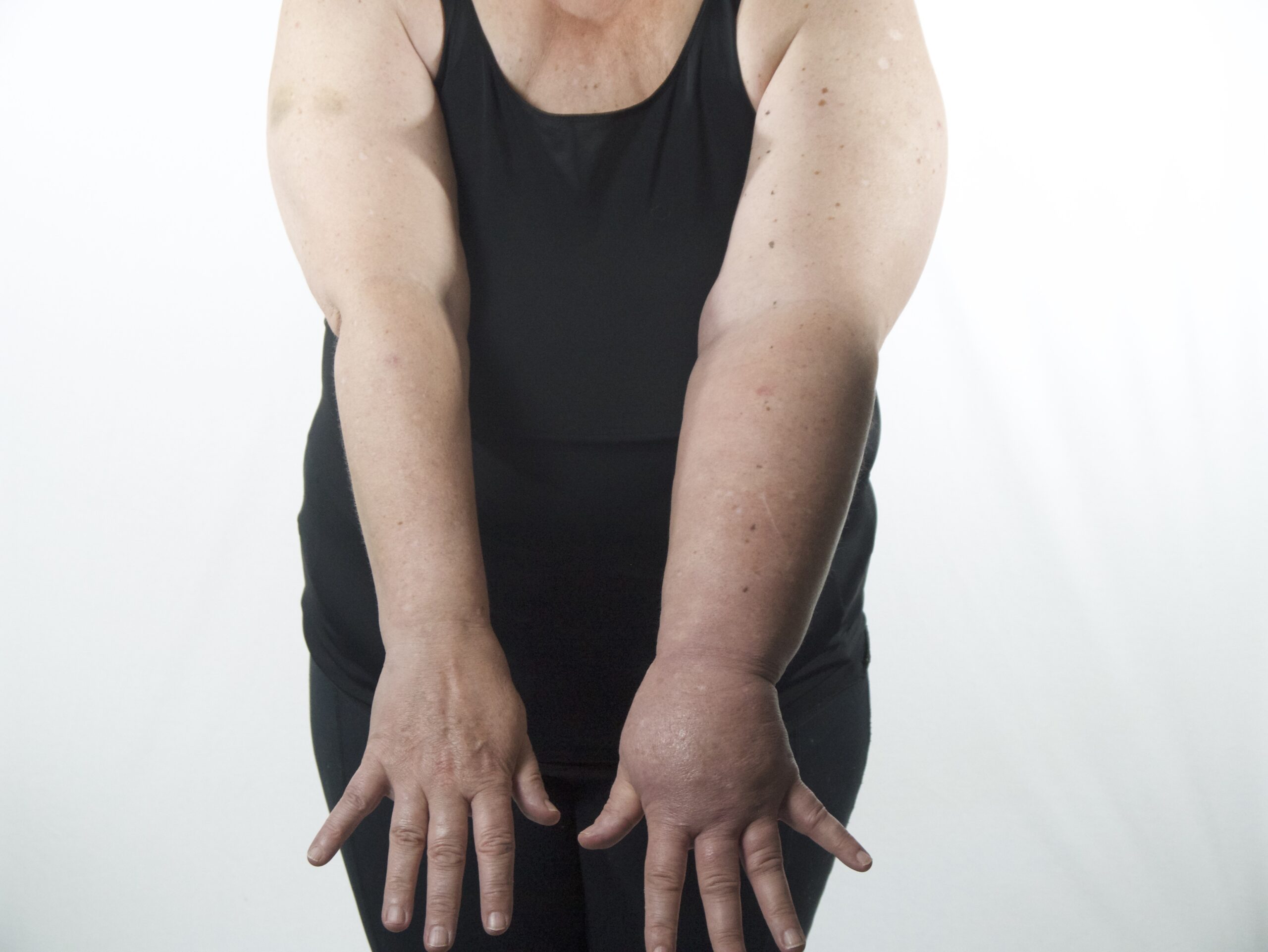
Lipedema vs Cellulite, Lipedema Stages and More

Diet for Lipedema
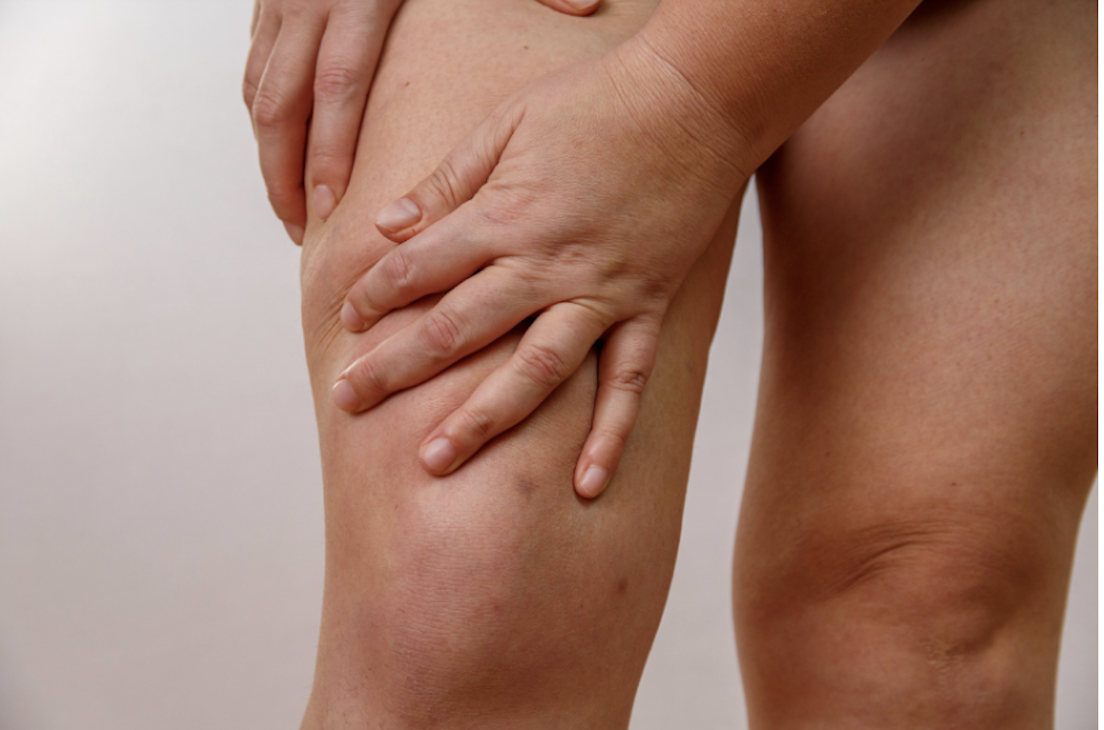
Lipedema Treatment
I’m a professional who walks alongside her clients with compassion. Right now, you’re facing a crisis…you’ve got cancer, lymphedema, lipedema or another issue that has got you wondering “what else can I do to help myself?” People around you are talking about diet, some of it sounds appealing, some of it sounds questionable, some of it sounds too good to be true…and you want to make sure you are doing things right. I can help.
I’ve helped my clients improve their cancer treatment side effects, improve their cancer-risk reduction diet, reduce their lymphedema, improve their lipedema pain and swelling. I can help you too.
When you work with me, you’re working with someone who has been there herself and lives in the real world. I’m not going to prescribe some overly restrictive protocol that is unsustainable. No meal plans. We will work together to evolve your diet to a sustainable routine that works for you and your family. We will set goals together and we will trouble shoot whats keeping you from achieving your goals.
Read my cancer story.
Compassionate, evidence-informed nutrition to support your treatment and recovery, from an expert who’s been where you are.
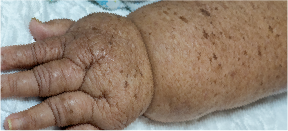
Nutrition solutions that support your lymphatic system, and are designed to reduce your swelling and pain and slow the progression of these chronic diseases.

Improve patient outcomes with research-supported nutrition therapies for lymphedema, lipedema and underlying inflammation.
Use nutrition to help you manage the side-effects of cancer treatment, then implement strategies to provide you with your best life after treatment. Use step by step complete decongestive therapies and nutrition to improve your lymphedema management and delay progression. Implement intermittent fasting to support a healthy weight, improved inflammation and other metabolic benefits.
Shop >